Have you recently been diagnosed with Type II Diabetes?
Are you worried that your diagnosis may affect your existing foot problems?
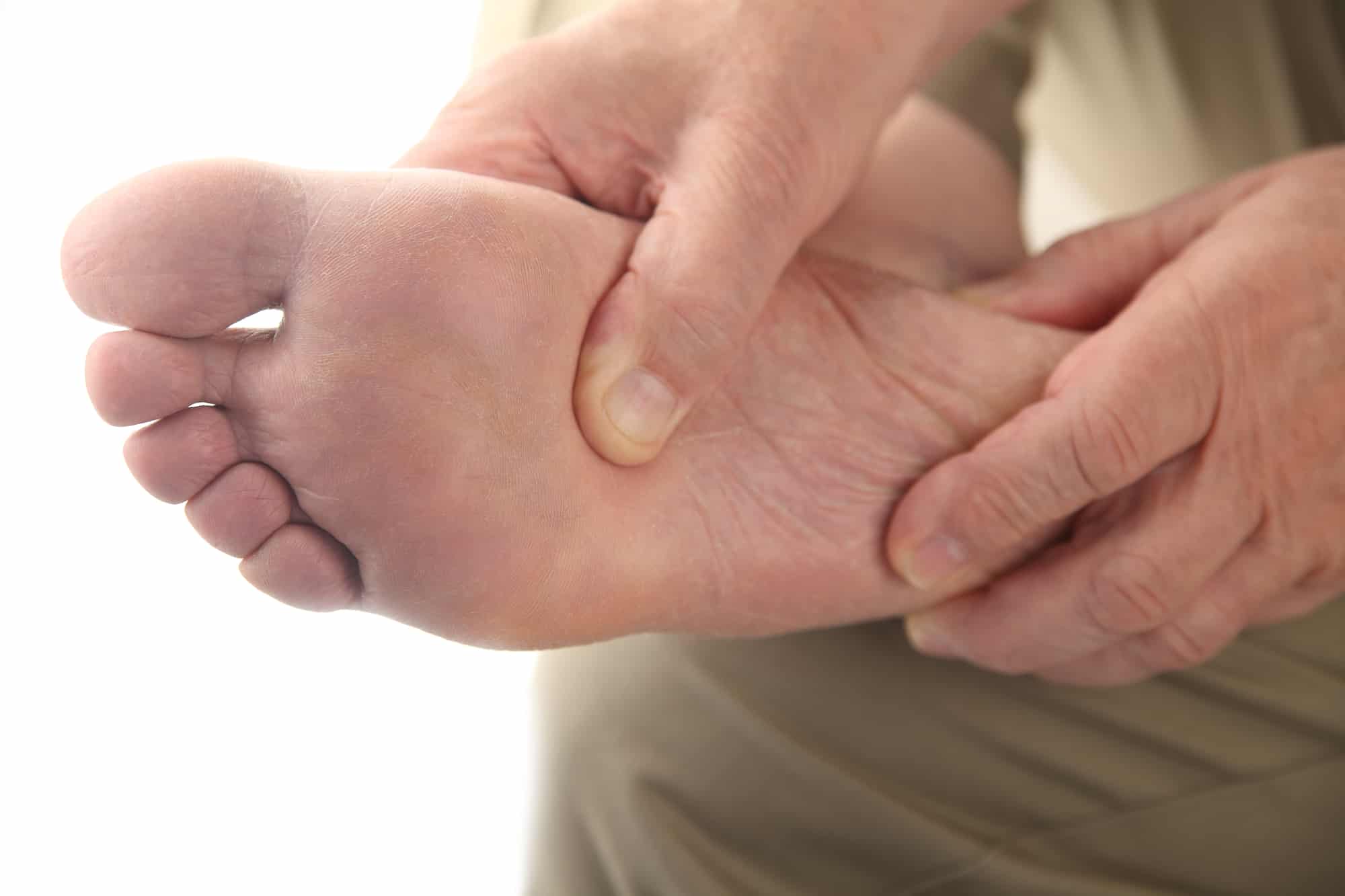
Diabetes is a disease that can lead to poor circulation, which can then reduce blood flow to the feet. This problem in circulation often causes ulcers and decreased sensation in the feet, making you more susceptible to foot pain and injury.
In addition to that, people who have diabetes sometimes don’t recover from foot injuries as quickly due to damage at the cellular level.
But don’t worry. We’re here to help.
Firstly, if you’ve just been diagnosed with diabetes, you’re not alone.
According to The World Health Organization and The WHO “Global Report on Diabetes,” world health experts consider diabetes a global epidemic. They estimate that by 2030 there will be 552 million people living with diabetes.
It’s a frightening statistic, no doubt about it. Plus, all those millions of people may also be affected by foot problems due to their diabetes, so it’s essential for us, as Physical Therapists, to examine the connection and educate those of our patients who have diabetes on how best to look after their feet.
The stats are an alarming wake-up call for us all. But for the individual – who doesn’t know about the condition, diabetes is also a scary diagnosis to receive.
Obviously – in an ideal world, the best way to avoid the negative health consequences of diabetes is to avoid getting it in the first place by making healthy eating and regular exercise part of your daily routine. But if it’s too late for that, all is not lost.
By making small, manageable changes to your lifestyle through diet and exercise, stress reduction, and sleep to control your blood sugar levels, it doesn’t have to be scary. Instead, it can be well managed in the case of Type II Diabetes – and the health problems avoided, if not wholly reversed (remission).
Physical therapy helps improve circulation by strengthening the muscles and joint tissues around the toes. It also helps maintain healthy gait patterns so that someone with diabetes is less likely to fall or slip on their way from one place to another. Physical therapy can also help improve sensibility in one’s toes to be less prone to injury by accidentally stepping on something sharp or harmful.
What is Type II Diabetes?
Diabetes is a chronic disorder that affects energy production in the body, specifically converting the food you eat into fuel for your cells.
When you eat carbohydrates, sugar, and to a lesser extent, protein, your body breaks these foods down into simple sugar molecules (glucose) that it then absorbs into the bloodstream. When your body senses this glucose in your bloodstream (which is measured when you check your blood sugar level), it tells your pancreas to make more insulin.
Insulin’s primary purpose is to help get the sugar (energy) in the bloodstream into your cells – to give you the power to walk, run, perform and face the day.
When the body deals with more glucose than it needs over a long period – from excess calories, carbohydrates, sugar, and little exercise, this process starts to malfunction. It begins with Prediabetes and insulin resistance.
When your blood sugar and insulin levels begin to move out of the upper normal range, ultimately, Type II Diabetes occurs.
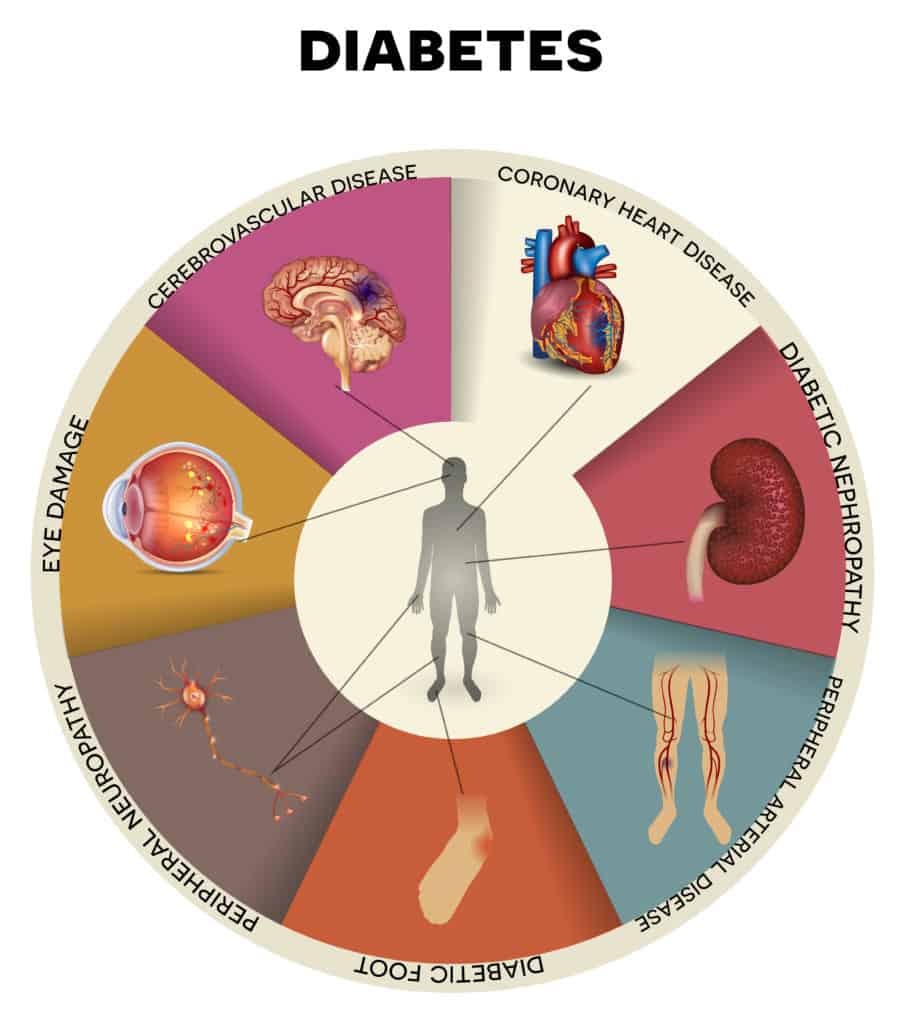
As a result of the excess sugar, the pancreas stops making enough insulin to regulate the blood sugar, and the cells stop responding in the same way. This breakdown leaves too much sugar left circulating in the bloodstream, which is the cause of diabetes-related health problems like heart disease, blindness, and kidney problems.
Diabetes and Feet: What’s the connection?

It’s a well-known fact that diabetes has a significant effect on your circulatory system. Also, the connection to the feet and problems with the extremities, such as open sores, fungal infections, and foot calluses, is prevalent in patients with diabetes. In rare cases – if patients don’t adequately control their blood sugar, the condition can eventually lead to severe disabilities such as blindness and amputations.
With Type II Diabetes, the body begins to develop insulin resistance. This change in how the body responds to glucose is called insulin resistance and is an early sign of diabetes. Until eventually, Type II Diabetes develops, and insulin does not move glucose from the blood into cells to store it for energy.
As a result, sugar builds up in the bloodstream and spills over into the urine. The cells are starving for fuel while too much sugar is stored in blood vessels and spilling over into urine from cells that cannot take it up as usual.
The glucose spills over into surrounding tissues and causes inflammation, nerve damage, and more problems with circulation throughout the body, including to the feet. This excess stored glucose causes diabetic foot disease (also known as a peripheral vascular disease).
Due to the impact of the big insulin spikes that occur after eating lots of carbs, followed by the “sugar crashes.” Sugar crashes are when you feel jittery and anxious as your blood sugar plummets to below normal levels in response to a high.
The fluctuating blood glucose levels and the effect on the circulatory system can cause damage to the blood vessels in your feet. One of the tell-tale signs of this is a pain when you rise on the balls of your feet, which you can test yourself at home. If you feel pain when you try this, we recommend you book an appointment with a Physical Therapist to have your feet evaluated.
Physical Therapy is a popular form of treatment for people who have diabetes who are looking to prevent diabetes-related foot problems. In recent years, this has led to an increase in physical therapists treating patients with diabetes. Physical therapy for diabetes reduces foot pain and improves your ability to do physical activities such as walking and climbing stairs.
As a result, you’re able to exercise more, which helps to regulate your blood sugar. This blood sugar modulating increase in activity is why regular physical therapists are less likely to suffer from diabetic complications; Such as nerve damage or heart disease.
One of the other negative health consequences of Type II Diabetes is Diabetic neuropathy. Painful diabetic neuropathy, or nerve damage, can make it difficult to walk or stand for long periods. It causes pain and numbness, mainly in the legs and feet, but it can also cause problems with the digestive system.
Physical therapy offers many benefits for people who have diabetes. It improves balance, helps with joint pain, and can even reduce the onset of diabetic neuropathy.
In addition, it can help reduce pain and stiffness caused by other common, co-occurring conditions such as arthritis or fibromyalgia. Studies have also shown that it can help people with diabetes lose weight and keep it off.
You can book a complimentary consultation with one of our Physical Therapists who specialize in diabetic foot care here.
The Physical Therapist’s Guide To Caring For Your Feet

If Physical Therapy isn’t an option for you right now, or you just want to take extra steps to help protect your feet between physical therapy appointments. There are lots of things you can do at home to look after your feet and prevent diabetes-related problems:
Check Your Feet
Have your feet checked over by your family physician at least once every 12 months. This annual check-up will pick up problems before they turn into something more serious.
Check your feet at home at least once per day. Make it part of your daily routine – either after your brush your teeth in the morning or right before you go to bed, it’s up to you. Look for any signs of ulcers, inflammation, callouses, or bruises.
Keep Your Feet Dry
This suggestion doesn’t mean that you can’t ever get your feet wet. Just make sure you dry them thoroughly after bathing, showering, or swimming and avoid spa treatments that require you to “soak your feet.” Also, pay attention to the areas between your toes that can get damp and harbor bacteria.
Moisturise Daily
With diabetes, it’s vital to prevent rough skin, peeling, and cracking on your feet as bacteria can penetrate through the cracks and broken skin, leading to infection. Make sure you rub the lotion in well, though, and don’t leave it lying on your feet.
Keep Toenails Short
Make trimming your toenails another part of your routine. We recommend using nail clippers to cut your nails and then use a gentle file to round the edges. This routine prevents ingrown toenails and other potential opportunities for infection.
Wear comfortable shoes
It’s crucial to wear cushioned and comfortable shoes or slippers at all times to prevent injuries to the bottom of your feet. With diabetes, your shoes are the most critical part of your outfit. Don’t be tempted to wear poorly fitting shoes.
Want to discuss your diabetes and foot treatments with a trained physical therapist? Get in touch with us anytime through our contact page!