I hate to say it but I have some scary news from Anthem Blue Cross.
Starting November 1, they will be utilizing a company called OrthoNet to authorize ALL physical therapy services.
Starting November 1, they will be utilizing a company called OrthoNet to authorize ALL physical therapy services.
This means even though you have a prescription from a physician, Anthem can (and will) deny your care.
We are able to evaluate you for your issue but then have to submit to OrthoNet for authorization of care… This will also cause delays in your care.
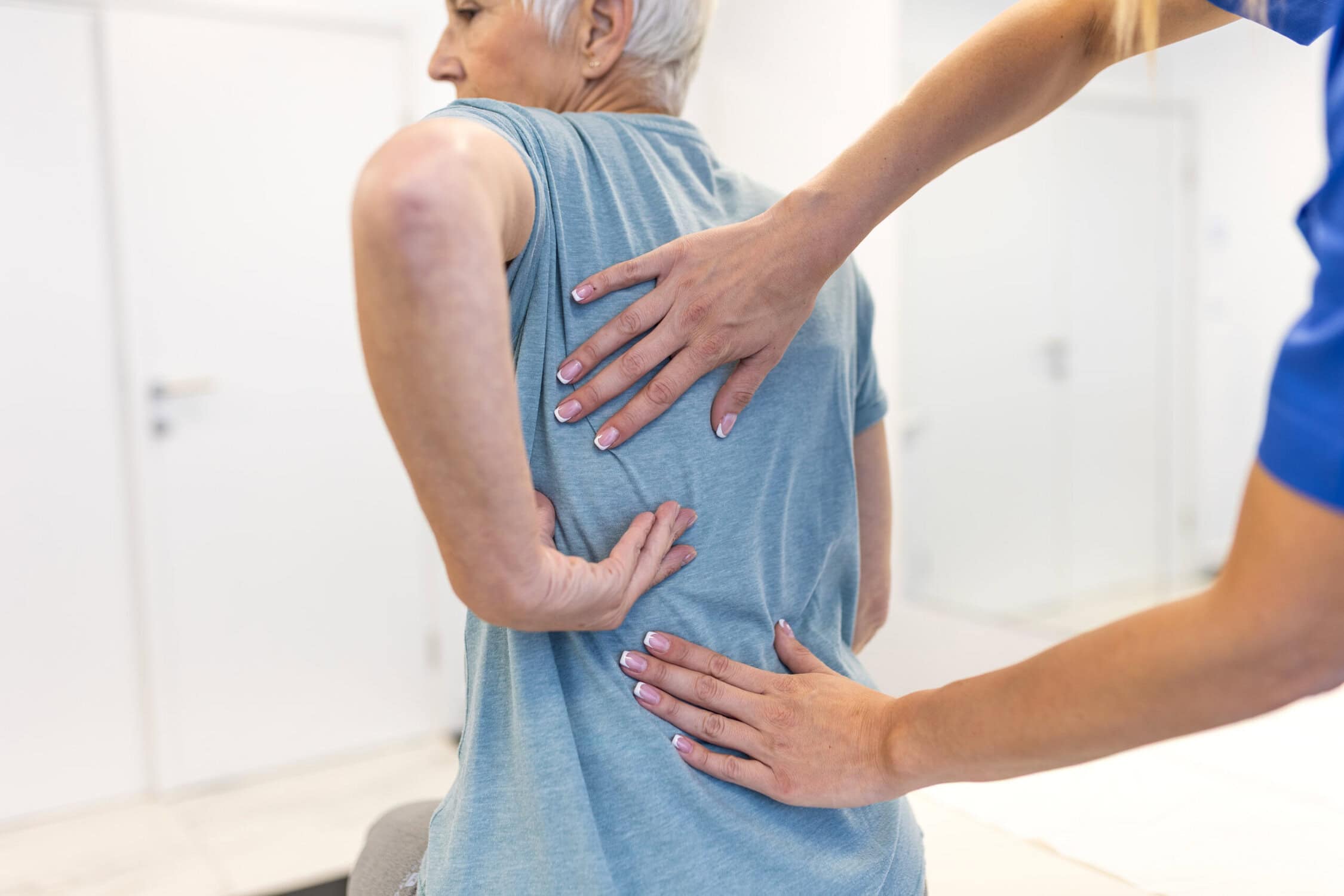
As a physical therapist I find this quite scary…someone sitting behind a computer screen (who might not even be a licensed physical therapist) is making the determination that you don’t need care.
If they do determine the care is necessary, they will only authorize 4 visits of care at a time.
Anthem says this is to control “claim trends” yet Anthem implemented financial control already back in 2010 when they changed reimbursement to a flat rate of $75 per visit. This slashed our rates by 40%. This flat rate is less than it costs me to have my doors open to treat you.
Anthem has been chastised by the State Insurance Commission for its ever increasing rate increases <<click this link to read the insurance commissioners press release>>, and is only concerned with its shareholders.
Can you help prevent this from happening? Yes you can! A phone call to Anthem and a letter to the State of California Insurance Commission can help.
As a physical therapist I find this quite scary…someone sitting behind a computer screen (who might not even be a licensed physical therapist) is making the determination that you don’t need care.
If they do determine the care is necessary, they will only authorize 4 visits of care at a time.
Anthem says this is to control “claim trends” yet Anthem implemented financial control already back in 2010 when they changed reimbursement to a flat rate of $75 per visit. This slashed our rates by 40%. This flat rate is less than it costs me to have my doors open to treat you.
Anthem has been chastised by the State Insurance Commission for its ever increasing rate increases <<click this link to read the insurance commissioners press release>>, and is only concerned with its shareholders.
Can you help prevent this from happening? Yes you can! A phone call to Anthem and a letter to the State of California Insurance Commission can help.
If you need m information, or clarification, please let me know!
Latest posts by Andrew Vertson (see all)